The Use of Hemodynamic Monitoring in Vascular Patients
C. O. Brantigan MD
A randomized prospective study is not required to prove that well
informed surgeons who are clinical physiologists will do better for
their patients than those who lack full respect for data available
for the asking in most modern hospitals ......Benfield, 1981 .
Patient Population Requiring Invasive Monitoring:
Patients with vascular disease that will benefit from hemodynamic
monitoring in the perioperative period are those who are critically
ill or who have metastable problems with their cardiac, cerebral or
renal circulations. Patients with aortic disease with comorbid
conditions and limb salvage patients are candidates because of the
high incidence of coronary disease and the high incidence of other
major medical problems.
Although these patients have a high incidence of diabetes,
hypertension, renal disease, chronic obstructive pulmonary disease
from smoking, pulmonary hypertension and polypharmacy, the impact of
coronary disease is the most studied of the comorbid conditions.
Coronary Artery Disease
Hertzer (1984) reported a series of 1000 patients with vascular
disease who underwent coronary arteriography. These were elective
vascular patients--neither those presenting significant coronary
symptoms nor those presenting as limb salvage candidates were
included. The procedures required were generally aortic or
femoropopliteal reconstructions.
Findings of Coronary Arteriography
Thus 92% of these patients had coronary disease. Limb salvage
patients have not been studied so systematically, but when they have
been studied, the incidence of severe coronary disease is even
higher. The prudent surgeon assumes that all of the limb salvage
patients and complex aortic reconstruction patients have significant
coronary artery disease. Hertzer believed that coronary
revascularization should precede vascular reconstruction, but the
mortality of the coronary therapy was greater than the vascular
procedure, and the only subgroup of coronary surgical survivors had
any long term benefit were non-diabetic men. All other groups showed
no increase in survival .
Peripheral vascular disease is a marker for increased mortality
independent of the coronary disease. The Coronary Artery Surgery
Study (CASS 1994) noted that markers of peripheral vascular disease
predicted a 25% increase in death rate for all groups (surgery or
not) at any point in time after controlling for other factors. Most
of these patients did not have vascular disease severe enough to
consider surgery, and were thus a healthier group than limb salvage
patients. Peripheral vascular disease is also an independent
predictor of death after coronary bypass. Patients with clinical and
subclinical markers of vascular disease in the data from the
Northern New England Cardiovascular disease Study Group experienced
a 2.4 fold increase in mortality and had a 73% higher chance of
dying during a hospitalization for coronary artery bypass (CABG)
than those without such markers. Survivors of the coronary artery
surgery died at an increased rate as well. Vascular patients
experienced a 20% mortality compared of 8% at 5 years. As a result
the authors questioned the role of CABG in these patients. Again,
this was not a group of patients with severe PVD, and thus
underestimates the problems faced by patients requiring surgery for
complex aortic disease or limb salvage.
As peripheral vascular disease patients go, those treated in our
practice are sicker than those seen by most vascular surgeons
because of the high incidence of limb salvage surgery in our
patients. This was strikingly demonstrated in the
multi-institutional study of Cryoveins that was reported at the
Society for Vascular Surgery in 1999 with Brantigan as the principal
investigator .
Physiologic Problems in Vascular Patients.
The importance of adequate intravascular volume, cardiac function
and appropriate vascular tone in vascular surgical patients has been
known for many years, and was discussed by Grow and colleagues in
the 1960's . Vascular surgeons have based their operations on
physiologic studies and have conceived of their perioperative
management in physiologic terms since vascular surgery became a
specialty. The most successful surgeons have always prepared their
patients well and have based their management decisions on
physiologic parameters. How is a patients cardiopulmonary physiology
best understood? Can it be accurately determined based on physical
examination and lab tests with the missing pieces assumed, or must
it be measured in some other way?
Brantigan (1980, 1982) studied the incidence of hemodynamic
abnormalities in the perioperative period, and characterized the
incidence and impact in 52 consecutive patients, predominately with
vascular reconstructions. There was no significant catheter
associated morbidity. The following abnormalities were observed:
| PAWP/CVP Discrepancies |
33% |
|
| Cardiac Performance Problems |
11.5% |
|
|
|
Along the way he noted that vasoconstriction led to a decreased
flow in the bypass grafts and an increased incidence of
perioperative thrombosis. The importance of flow in keeping bypasses
open is a well known phenomenon. During that time period hypothermia
and common use of vasoconstricting antihypertensives such as
thiazide diuretics and beta blockers were important contributing
factors that have been ameliorated by having temperature control in
the operating room and by the newer antihypertensives. Brantigan
characterized the impact of invasive monitoring on these patients as
follows:
|
|
|
|
| Helpful (less worry for physician, less
calls at night etc) |
19% |
|
| Therapy change mandated by measurements
|
37% |
|
| Potentially life saving change in therapy
|
27% |
|
Del Guercio reported similar studies on 75 routine vascular
patients with the similar results in 1982 . Unlike Brantigan, he
included preload problems predictable using just a CVP, but found
the following abnormalities:
| Normal Hemodynamics |
33.3% |
|
|
|
|
|
|
|
| Combination of above |
9.3% |
|
While certainly some physicians are more skilled in the intuitive
assessment of their patients, and some anesthesiologists are more
able to tune patients hemodynamics during the early stages of an
operation, many studies over time have documented that in high risk
patients details of their physiology can not be accurately estimated
without direct measurements. It is not possible to distinguish
patients who are volume depleted from those who need inotropic
support of vasodilation for optimization on clinical grounds alone.
The question "does it matter," strikes at the very core of the
theoretical underpinning of what we do as vascular surgeons.
Hemodynamic Tuning Algorythm
Based on these data, Brantigan began to admit patients to the ICU
for preoperative tuning if they were sick aortic patients or were
limb salvage patients. They were tuned using the following
algorithm:
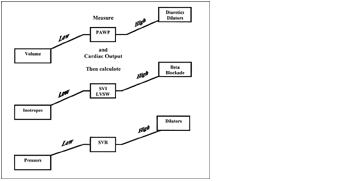
Preload was adjusted first using volume loading or diuresis and
vasodilators. Attention was then turned to the LVSW and SVR and
these were adjusted. On the diagram above the high LVSW is included
to balance the diagram--the only time this is seen is in delirium
tremens, thyroid storm and occasionally in acute myocardial
infarctions. It is acknowledged that balancing these factors is like
balancing the legs of a three legged stool, and that repeated
modifications are needed as the adjustment of one parameter affects
the other.
The goal is to send a patient to the operating room with a
cardiac index of >2, a SVR of about 1000 and a PAWP optimized based
on urine output and cardiac output. Patients commonly are taken to
the operating room on a nitroprusside drip or a nitroglycerin drip.
Inotropes are not unusual, and even patients with bad ejection
fractions can be well managed if their cardiac index can be easily
kept above 2 with a combination of inotropic support and
vasodilation. The strategy is to achieve cardiopulmonary function
sufficient to tolerate the operation. The strategy of maximizing
cardiac function has been proven detrimental.
Most anesthetics vasodilate particularly epidurals, which are
particularly advantageous for vascular patients, as they maximize
flow thru the grafts during the perioperative period. As the
anesthetic is dialed in preoperative nitroglycerine or nitroprusside
are dialed down. As the patient recovers from anesthesia the process
is reversed. Distal bypass patients are then switched to oral
medications to maintain the same parameters in much the way that
cardiologists use what Braunwald characterized as "tailored therapy"
for heart failure patients. In patients with significant third space
losses and compromised cardiac function, patients are kept in the
ICU until they demonstrate their ability to handle fluid as they
mobilize it.
Results
Compared with published series, our patients have comparable
success rates, but the incidence of unfavorable anatomy is higher
and the patients are sicker, as judged by their higher long term
mortality.
Brantigan discussed this strategy at Wound Care Center National
meetings and David Knighton then studied the effect of this
treatment strategy on distal bypass patients. His was a randomized
trial of the effect of preoperative tuning on the outcome of limb
salvage surgery in 89 patients and was published in 1991 . Excluded
were patients who:
- Had a MI within the last 3 months
- Had a CABG within the last 6 weeks
- Had clinical congestive heart failure
- Had unstable angina
All patients were operated upon by the same surgeon and all had
anesthesia administered using identical techniques. End points for
tuning were:
PAWP 8-15 mm Hg
CI >2.8
SVR <1100
Of the patients tuned:
36.8% met criteria without intervention
26.4% required volume loading alone
36.8% required inotropes and or vasodilators with or without
fluid loading
The patients tuned before surgery had fewer adverse events during
surgery, less cardiac morbidity, less early graft thrombosis and a
lower mortality (1.5% vs. 9.5%) (All p<.05). There was no increase
in ICU LOS, hospital LOS, hospital costs compared to controls. The
per cent of hospital costs attributed to complications was higher in
the control group. Note that this is a study not of Swan Ganz
catheters, which would be inappropriate, but rather is a study of a
management strategy based on hemodynamic parameters.
Preoperative Tuning or the Importance of Early Intervention
The importance of preoperative hemodynamic tuning or at least
early intervention in high risk patients has been emphasized
repeatedly. This is particularly true in aortic reconstructions.
Shoemaker, in a widely quoted randomized study , established
physiologic goals for management of high risk patients and then
studied the effect of achieving these goals during the perioperative
period. The goals were achieved in 68% of patients by volume
adjustment, 25% by adding dobutamine and 7% by adding nitroprusside
in a strategy similar to the algorithm above.
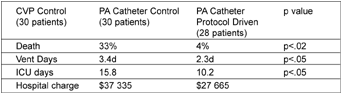
Although the control patients with a pulmonary artery catheter
experienced a 25% decrease in mortality the other variables were the
same between patients managed using the CVP catheters and pulmonary
artery catheters. Clearly the therapeutic strategy made the
difference. Insertion of a catheter is not therapy.
Shoemaker concluded, "...most surgical patients do rather well.
Overall mortalities of less than 2% in major surgery are usually
considered acceptable in most hospitals. Hence, most surgeons are
unwilling to depart from their well-organized routines until it is
obvious that something has seriously gone wrong. By this time,
lethal postoperative complications may already have begun, and it is
too late for early, much less prophylactic, therapy. Preoperative
identification of high risk patients and the use of prophylactic
monitoring to optimize circulatory function generally have not been
accepted. Moreover, the concept has been only slowly appreciated
that the high risk patient could be identified before surgery by
clinical criteria [read hemodynamic criteria] and that the majority
of surgical deaths and organ failures could be prevented by
prophylactic therapy that augmented compensatory responses to tissue
hypoxia." At one point during his series of studies, an
institutional decision was made to ban preoperative inserting of
Swan-Ganz catheters. The death rate returned to control levels and
the same number of Swan-Ganz catheters were used in the end, but to
treat problems rather than to anticipate them. Boyd and Hayes also
emphasized the importance of early intervention. In a meta analysis
of six randomized studies of hemodynamic paramater driven therapy
they found significant outcome improvement in high-risk patients
with early therapy directed to achieving optimal goals .
Many studies have emphasized the importance of volume loading in
preparation for aortic surgery . This is best accomplished
preoperatively using hemodynamic monitoring. With monitor guided
volume loading the incidence of hypotensive episodes is decreased,
renal dysfunction is decreased and mortality decreases as well (Hesdorfer
et al 1987) . None of the other strategies of renal protection, such
as administration of mannitol, lasix or ACE inhibitors has been as
effective. Bertolissi (1998) in discussion prevention of renal
failure in major vascular surgery emphasized that "Optimal
management of the cardiovascular function by means of invasive
hemodynamic monitoring is the main tool to protect the kidneys and
prevent renal failure" in vascular patients. Preoperative
preparation is better than catch up during surgery. Amin and Iberti
described why that would be in 1990 and the principles are true to
the present:
- "Despite what is frequently published, every medication,
especially the inotropes, may have markedly different effects in
different patients."
- "Commonly the initial hemodynamic profile does not reflect the
patient's true baseline due to anxiety and stress, and a longer
period of time may be required" for an adequate understanding of
the patients physiology and response to interventions.
- "Contrary to the maximization philosophy (attempting to
achieve the highest possible cardiac output), it is a better
approach to have the patient meet his/her oxygen requirement using
the least possible cardiac work." and this takes time.
In recent years there has been an increasing call for a
randomized control trial of the Swan Ganz catheter. Some
investigators have insisted that there be a moratorium on the use of
these catheters until their use is validated by such a trial.
Insertion of a Swan Ganz Catheter allows acquisition of data.
Acquisition of data, per se does not change outcome unless either
there is morbidity associated with the acquisition of the data or
the data is used to direct therapy. Morbidity associated with
insertion and maintenance of the catheter should be minimal assuming
competent intensivists and nursing staff. Most of the morbidity of
hemodynamic monitoring results from either a lack of understanding
of the data or its misapplication. Attempts to determine the
competence of physicians using hemodynamic monitoring have been
disappointing. When standardized testing of basic knowledge have
been given, one third to one half of the questions have been
answered incorrectly . That level of misunderstanding is a
credentialing problem that is nationwide. Studies noted above
validate the management strategies described above.
Conclusions
The importance of preoperative preparation of a patient for major
surgery has been known for many years. The concept is taught in
medical school. The concepts were discussed in the American College
of Surgeons Manual of Preoperative and Postoperative care in the
1960's . Invasive monitoring allows us to measure and quantify the
physiology that we are trying to modify. Used accurately and
thoughtfully in the appropriate patient, this strategy decreases
mortality and morbidity and increases graft patency.
Dr Brantigan wrote this article in December 2001.
References:
1 This quote is from a reliable source--my slides.
I cant for the life of me find the original source. It has to be
from a discussion of monitoring in aortic surgery.
2 Hertzer, N et al, Coronary artery disease in
peripheral vascular patients, Ann Surg (1984) 199:223-233.
3 Hertzer, N, discussion in Cutler, BS, Leppo, JA,
Dipyridamole thallium 201 scintigraphy to detect coronary artery
disease before abdominal aortic surgery, J Vasc Surg (1987)
5:91-100.
4 Eagle, K, Rihal, CS, Foster, ED et al, Long-term
survival in patients with coronary artery disease: Importance of
peripheral vascular disease, J Am Coll Cardiol (1994) 23:1091-5.
5 Birkmeyer, JD et al, The effect of peripheral
vascular disease on in-hospital mortality rates with coronary artery
bypass surgery. Northern New England Cardiovascular Disease Study
Group. J Vasc Surg (1995) 21:445-52.
6i Brantigan, CO et al, Revascularization of the
Lower Extremity with Cryopreserved Saphenous Vein: a Multicenter
Clinical Experience, Poster Session, International Society for
Cardiovascular Surgery, Washington, DC, June 1999.
7 Wilson, J.N., Grow, J.B., Sr., Demong, C.V.,
Prevedel, A.E., Owens, J.C.: Central Venous Pressure in Optimal
Blood Volume Maintenance. Arch Surg 5:55, 1962.
8 Symposium on Hemodynamic Monitoring, Denver CO,
March 28, 1980.
9 Brantigan CO, Hemodynamic monitoring: A technique
for critical care nurses. Am J Nurs 82:86-89, 1982.
10 Babu, S, Sharma, P, Raciti, A, Mayr, CH, Elrabie,
NA, Clauss, RH, Stahl, WM, DelGuercio, LM, Monitor-Guided responses;
operability with safety is increased in patients with peripheral
vascular diseases, Arch Surg (1980) 115:1384-86.
11 Braunwald, E, Heart Disease, WB Saunders,
Philadelphia 1997 p 508.
12 Berlauk, JF, Abrams, JH, Gilmour, IJ, O'Connor,
SR, Knighton, DR, Cerra, FB, Preoperative optimization of
cardiovascular hemodynamics improves outcome in peripheral vascular
surgery, Ann Surg (1991) 214:289-299.
13 Shoemaker, WC, Kram, HB, Appel, PL, Fleming, The
efficacy of central venous and pulmonary artery catheters and
therapy based upon them in reducing mortality and morbidity, Arch
Surg (1990) 125:1332-8.
14 Boyd, O, Hayes, M, The Oxygen trail: the goal Br
Med Bull 1999;55:125-139.
15 Grindlinger, GQ, Vegas, AM, Manny, J, Bush, HL,
Mannick, JA, Hechtman, HB, Volume loading and vasodilators in
abdominal aortic aneurysmectomy, Am J Surg (1980) 139:480-6.
16 Whittemore, AD, Clowes, AW, Hechtman, HB,
Mannick, JA, Aortic aneurysm repair; reduced operative mortality
associated with maintenance of optimal cardiac performance, Ann Surg
(1980) 192: 414-21.
17 Hesdorfer, CS, Milne, JF, Meyers, AM, Clinton,
C, Botha, R, The value of Sawn-Ganz catheterization and volume
loading in preventing renal failure in patients undergoing abdominal
aneurysmectomy, Clinical Nephrology (1987) 28:272-6.
18 Bertolissi, M, Prevention of acute renal failure
in major vascular surgery, Minerva Anesthesiol (1998) 65: 867-877.
19 Amin, D, Iberti, TJ, Use of the surgical
intensive care unit in the preoperative preparation of the high risk
patient, J Cardiothoracic Anesthesia (1990) 4: Suppl1, 13-18.
20 Iberti, TJ, Fischer, EP, Leibowitz, AB, Panacek,
EA, Silverstein, JH, Albertson, TE, and the Pulmonary Artery
Catheter Study Group, A multicenter study of physician's knowledge
of the pulmonary artery catheter, JAMA (1990) 264:2928-32.
21 Randall, HT, Hardy, JD, Moore, FD, Manual of
preoperative and postoperative care, American College of Surgeons,
WB Saunders, 1967. |